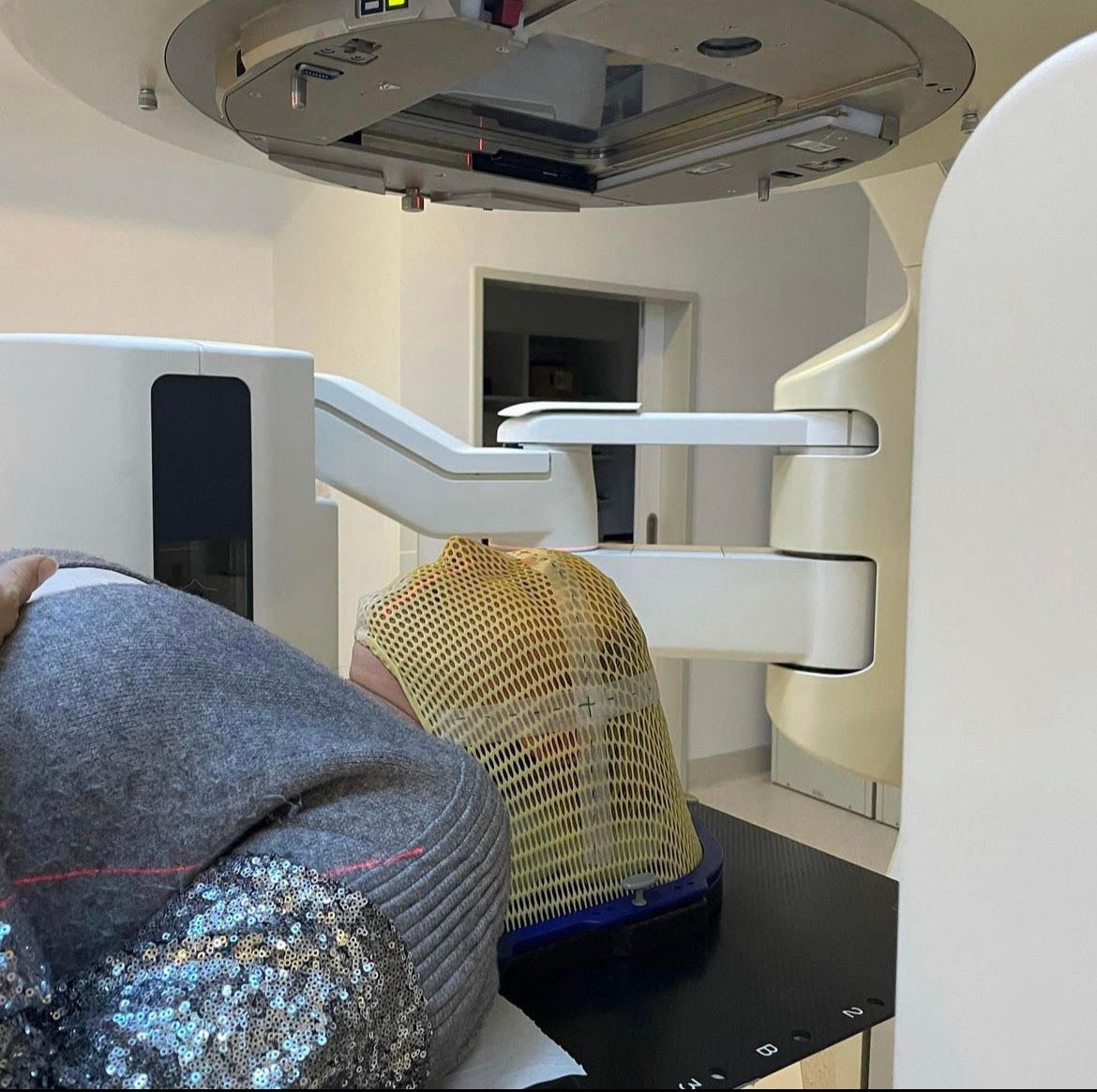
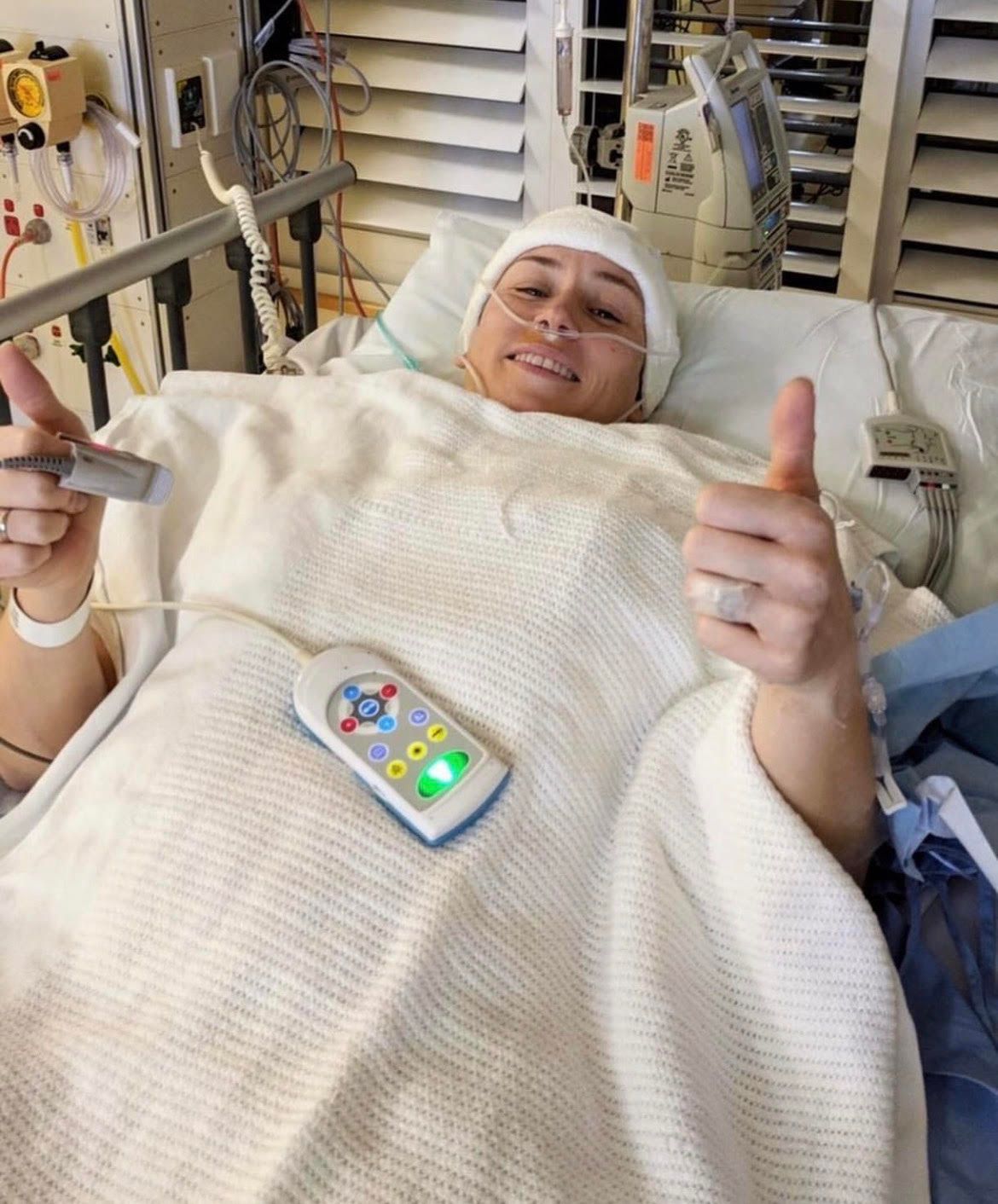
Prior to the bout of pneumonia that led me to seek treatment for a persistent and unrelenting headache, I was a busy and dedicated middle manager, working for a large property group. I had grown used to the dull pain behind my eyes and persistent headache. At 38, I was far too focused on work, life, and career advancement to pay it much attention. But after a few months of the ongoing headache, I booked to see my GP. Immediately she recognised the symptoms of a brain tumour.
At the time, my children were 6 and 4. So, the diagnosis was… unwelcome, to say the least.
Within a week my medical team swelled from a GP taking care of my pneumonia and headaches to including a medical oncologist, a neurosurgeon, a psychologist, and not one, but two, radiation oncologists.
Generally, medical experts cannot tell a patient how long a tumour has been in the brain, but in my case, it was clear, the tumour had been growing for years. By the time I was diagnosed it had infiltrated most areas of the brain and had started causing silent seizures that resulted in persistent confusion, short-term memory loss, and numbness along my right side.
The trick with slow-growing brain tumours is that the brain often finds ways to work around its uninvited squatter. Like flowing water taking the path of least resistance, the diffused tumours often grow around the critical infrastructure of your brain. In turn, the brain can do an amazing job of creating new pathways to carry out the day-to-day work, while contending with the intrusion.
Initially, I was devastated. Facing a terminal diagnosis raises the question, how do you measure if a life has been well lived? Is it achievement? Money? Output? Overcoming adversity? Did I work too much and achieve too little? How well can these final years be lived? How can I protect my children? How will they remember me?
The adage is that we live one day at a time – but surely that day is driven by what you intended to do the day after? I do not know the answers to these questions, but it has driven me to live as best I can under the circumstances.
I threw myself into a project that has become The Survivorship Diary, a resource for patients to help manage their medical information and record the various stages of treatment. I found this project to be cathartic, and I felt like I, might be helping other patients and their families.
In the 4 years since diagnosis and treatment, I have become calmer, finding some stability in this unexpected space. Knowing my life might be shorter than the average, has led me to better engage with the family.
I am more emotional than I used to be. I now have the time to empathise with the other people around me, and this has allowed me to build stronger relationships. Now I find joy in the humdrum of family life – the school drop-offs and pickups, sports, and night-time stories. While the years might be numbered, there is a new opportunity – a new and improved role in the family – one I didn’t know I needed until it was here.
I know I can’t expect a long lifetime, but I am thankful for the time I do have.